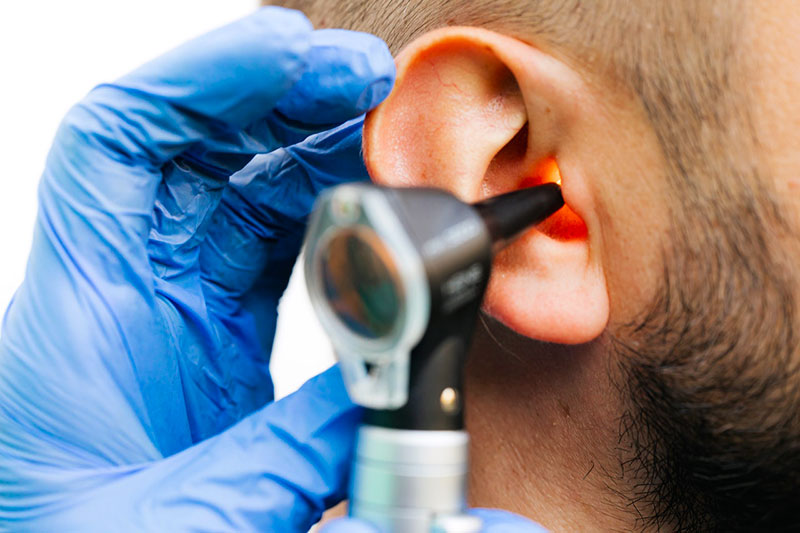
Perichondritis is the condition where the skin around the perichondrium of the ears becomes inflamed or infected. The perichondrium is the area of fibrous connective tissue found between bones and joints. The skin surrounding the ears’ perichondrium is called the pinna. When this area becomes infected or damaged, it can lead to recurring issues if not treated properly. This condition results typically from wounds such as ear piercings, insect bites, burns, and surgeries. People with compromised immune systems or inflammatory disorders are more likely to develop and suffer from reoccurrences of perichondritis.
Commons Signs and Symptoms of Perichondritis
People suffering from perichondritis report experiencing:
-Swelling and redness of the ear
-Earaches and pain around the area
-Infections, abscess, and production of puss
-Body aches, pain, and fever
In severe cases, the infection can spread to other areas in the body, worsening symptoms.
Treatment Options for those Suffering from Perichondritis
Perichondritis is a complicated issue with many variables; in the end, a medical specialist must evaluate and create an adapted treatment for each case as it is presented. The severity of the condition has to be considered as well as the overall health of the patient. Sometimes a culture has to be taken to determine how nasty the infection is. For mild bacterial infections, oral antibiotics will clear up the symptoms. Removal is required for cases involving a foreign object, like splinters or an abscess. In extreme cases, antibiotics can be given intravenously, or hospitalization may be suggested. Once an infection becomes genuinely awful, it can affect the tissue in the area and cause damage to cartilage and other soft tissues. While a rare occurrence, only a certified plastic surgeon can remedy deformations that result from advanced perichondritis. It is vital that doctors and patients need to understand the facts associated with perichondritis to determine the best treatment.
Frequently Asked Questions
Perichondritis is an inflammation or infection of the skin around the perichondrium, a layer of fibrous connective tissue found near the ears' cartilage. It primarily affects the pinna, which is the visible outer part of the ear surrounding the perichondrium.
Common symptoms of perichondritis include swelling and redness of the ear, earaches or localized pain, infections that may lead to abscesses and pus production, as well as systemic symptoms like body aches, pain, and fever. In severe cases, the infection can spread and worsen symptoms.
Perichondritis typically results from wounds or injuries to the ear such as ear piercings, insect bites, burns, and surgeries which may allow bacteria to infect the area. Individuals with compromised immune systems or inflammatory disorders are at higher risk of developing and recurring perichondritis.
Diagnosis and evaluation of perichondritis require a medical specialist who assesses the severity of the infection and the patient's overall health. Sometimes, a bacterial culture is taken to identify the specific infection. This evaluation helps guide appropriate treatment strategies.
Treatment depends on the severity of the infection. Mild cases are treated with oral antibiotics, while infections involving foreign objects or abscesses require removal. Severe cases may need intravenous antibiotics or hospitalization. In advanced infections causing cartilage damage, plastic surgery might be necessary to correct deformations.
Yes, if perichondritis is severe and left untreated, it can damage the cartilage and soft tissues of the ear. This damage can lead to deformities that might require plastic surgery to correct. Prompt medical attention is crucial to prevent such outcomes.
Individuals with compromised immune systems or those suffering from inflammatory disorders are more susceptible to developing perichondritis and experiencing recurring infections. This increased risk is due to a decreased ability to fight off infections effectively.
